Born too soon
It’s World Prematurity Day – one of the most important days in the year to raise awareness of the challenges and burden of pre-term birth globally. Amanda Eulenkamp reports on the local situation...

WORLDWIDE more than one in 10 babies are born too soon – and every one of these tiny miracles deserves a chance to survive, thrive and be happy.
Sadly, being born prematurely is the main cause of death in children under five world-wide.
Approximately 60 babies each year benefit from the love, care and attention of the medical staff at the PEH’s neonatal unit. Part of Frossard Ward, the unit becomes the home and focus of these babies and their families for as long as they need.

There are three cots in the unit, usually occupied by a premature baby, but also occasionally used for full-term babies who are not healthy. It’s a stressful time for the families involved, but they are supported by a fabulous team of paediatricians and nurses.
‘You can have a healthy premature baby or a sick premature baby,’ said senior neonatal nurse Jackie Smith. ‘When you have a healthy premature baby, it’s fear of the unknown for the parents. Our role includes putting the parents’ minds at rest about prematurity, especially when the baby is healthy. Obviously, things can go wrong, but we take it one day at a time.
‘But when you’ve got a sick and premature infant, that’s a totally different scenario. It’s incredibly stressful. They need all the support they can get. That’s why the Priaulx Premature Baby Foundation (PPBF) is important.’

Priaulx Premature Baby Foundation
PPBF was set up by three-times World Touring Car champion Andy Priaulx and his wife Jo. Both of their children (Seb, now 19, and Dannii, who is 17 today) were born prematurely. Dannii was born in Guernsey and was in the neonatal unit. The couple set up the foundation because they wanted to give something back to help other families in the same situation.

The PPBF – whose trustees, in addition to Andy and Jo, are Richard Le Tocq and Guy Hardill – have supported around 800 premature or seriously ill children and their families and raised almost £1m. locally. They’ve helped the Guernsey neonatal unit by providing specialist equipment such as state-of-the art incubator units, a jaundice diagnostic machine and a resuscitation baby doll for training.
As well as a support network, PPBF provides baby boxes for the newborns. These include soft muslins (‘much softer than rough hospital sheets’) and a ‘Cuski’ comforter. Cuskis are used by many neonatal units around the world. The idea behind them is that they are scented with (usually) the mother’s smell so that the baby can have it by them, helping bonding when the parent cannot physically hold them. ‘They also supplied us with a printer, so that when the baby’s first admitted and settled in, we can take a picture for the parents. A picture says a thousand words,’ said neonatal nursery nurse Emma McKane.
PPBF has also provided cool bags for the mothers to store their expressed milk in if they’re at home, then bring it back to the ward and pop it into the fridge.
Emma also tests the baby’s hearing before they go home, using equipment bought by the PPBF. ‘We also do a lot of parent craft – showing the parents how to bath the baby, help with any feeding issues, and also helping them get into their car seats as some premature babies are too small for them.’

As well as practical nursing, Jackie, Emma and the team are available to spend time with the parents. ‘Because we can only take three babies, and we’re a small unit, we get to know the parents very well,’ said Jackie. ‘It’s not always about their pre-term baby, sometimes they just want a bit of distraction. We recognise the non-verbal communication; you can gauge if there’s something troubling them.’
The ongoing support of the foundation is vital to the neonatal unit providing the extras that the hospital can’t at the start of life – and the medical staff are eternally grateful to them.
Priaulx Premature Baby Foundation Trustee Guy Hardill said: 'We are fortunate at PPBF to own two flats outright in Southampton, which offer comfort to Bailiwick families in times of great stress.
'Owning two properties comes with overheads, however, we have been delighted with the support from the Lloyds Bank Foundation for the Channel Islands and the Guernsey Community Foundation.

'With the grands from these foundations we have been able to meet the running costs of the flats and continue to support the Princess Elizabeth Hospital and offer support to those families whose babies have required time with the neonatal unit by the issuance of special baby boxes.
'No charity should rely or become dependent on such grants, it is our fiduciary responsibility to take the respite and use our time and efforts to seek long term support, which we are actively doing.
'2020 has seen the loss of a multitude of planned events and associated fund raising. Grants such as these are priceless to maintain the charity and ensure our work in the Bailiwick community continues for decades to come.'

Paediatric care
Dr Clare Betteridge is one of five consultant paediatricians on the island, who between them look after all the children who need medical care. She talked about the importance of the neonatal ward and the PPBF.
‘The neonatal unit takes babies from around 32 weeks and upwards. We will sometimes take them a little bit earlier, and they’ll stay here for as long as they need.
‘We also look after babies who have been born earlier than that in the UK – they’ll be repatriated here when they’re ready.

‘The babies can have most of their investigations here and we liaise with other specialists in the UK. If a baby is seriously ill or has a condition that we can’t treat on-island, we will transfer them with a specialist neonatal team over to (usually) Southampton, but we do try and do as much as we can here.
‘The main reason the Premature Baby Foundation is important is that people feel very alone when they’ve had a prem baby. Luckily, we’re OK here at the moment with Covid, so people are allowed to visit at any time.’
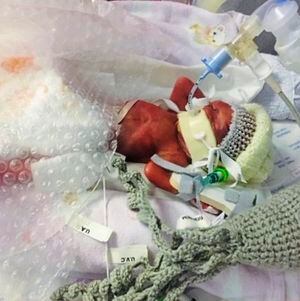
Dr Betteridge added that if a baby goes over to Southampton, they could potentially be there for weeks. ‘For the person going with them, they could be away from family, friends, pets, their homes and other children for a long time.’
PPBF has two flats in Southampton – Aggie’s Burrow and Isaac’s Pad – which are a godsend for parents who can live in them in privacy during the often-traumatic time their baby is in hospital.
One family which used Aggie’s Burrow for a number of months was the Morgans, whose baby, Zara, was born at 24 weeks.

What it’s like to have a premature baby
Alexis and Gareth already had a son, five-year-old Jasper, when their daughter was born. She was expected to arrive after his sixth birthday but was actually born at just 24 weeks.
‘Having a premature baby is not something you expect to experience and you can’t really prepare for it,’ said Alexis.
At 23 and a bit weeks pregnant, Alexis just ‘felt something was wrong’. Luckily for the couple, her mother had retired and was able to take Jasper, leaving them free to head up to Loveridge Ward.

However, things spiralled once she’d been seen on the ward, and they were off to Southampton on the next plane.
Handling this worry would be enough for anyone, but they had to explain to Jasper what was happening. ‘I told him that the baby needs to stay in Mummy’s body, and it wants to come out. But it’s not ready to come out yet, but if it does come out, all the right doctors and nurses are here to look after it the best they can,’ said Alexis.
She and Gareth had hoped to be able to go to 30 weeks, but complications arose, and Zara was born.

‘Jasper’s first question was: “Is it going to survive?”, which was extremely hard,’ said Gareth. ‘We didn’t pull any punches because we didn’t ever want to lie to him and give him false hope. So, we said “We very much hope so, but we don’t know”.’
Alexis said that when her mum brought him over when Zara was a week old, he was so proud of her.
‘She was very sick then and we didn’t know whether she was going to survive,’ said Alexis. ‘But we tried to give him things to celebrate in case that was going to be his memory of having a sibling. We got a M&S cake – and we were in Aggie’s Burrow at that point.’
The couple said that having the PPBF flat was ‘fundamental to making Jasper’s life over those four months that we were in the UK cosy and “normal”, and not distressing’.

They even decorated the small single room with bunting with his name on and bought a tree and decorations at Christmas.
A little lioness
‘When you have a premature baby, because you feel like you have one job to do – and that is to grow your baby – you feel like you’ve let it down,’ said Alexis. ‘It’s really hard to watch them because as any parent of a sick child would say, if you could put yourself in their place, you would. All you can do is hold them and be there for them. And I guess that’s another reason why Aggie’s Burrow was invaluable, because it is so close to the neonatal unit.
‘I could give myself to her every single waking moment.’
Tiny Zara – whose name means blossoming – proved to be a fighter. ‘She was doing the tough stuff,’ said Alexis.
Now safely back home with her loving parents and proud big brother, Zara needs to have regular follow-ups. But she continues to fight and continues to live up to the meaning of her middle name, Arielle – lion.
Alexis and Gareth's tips to parents
'I failed so much to follow this advice,' said Alexis. 'But take each day at a time. I worried so much about her future and the effects on her of such an early birth. I worried about the effects of what our family life was going to look like and the effects on Jasper.'
Don't be afraid to ask questions: 'When you walk into the neonatal unit, it's the adults who are shocked by the wires and the noises and how overwhelming it can look. The babies are just little sticks and skin and bones, and they are so fragile. Their skin isn't quite ready so you can't touch them. The nursing staff in Southampton were so great at explaining everything, whether you ask or not.'
Don't be afraid to get involved in your baby's care. 'It took me a while to get comfortable changing her nappy,' said Alexis. 'Sometimes it became like defusing a little bomb.'
Containment holding - 'We were shown how to gently cradle her head and her feet. It makes the baby feel secure, almost like being back in the womb. The nurses make a little nest around them to make them feel contained - that also helps with their limb development when they start to move a bit more. I held her, and held her, and held her,' said Alexis.
Don't be self-conscious - 'I felt so self-conscious singing to my little baby in her plastic box or reading a book out loud in a room where there are potentially six other parents. But it's the best thing ever and actually, eventually, everyone's doing it. That's brilliant.'

If you would like to make a donation big or small, or have any fundraising ideas, they would be gratefully received. Get in touch with sammy.meerveld@ppbf.org.gg.
Go to the new PPBF website: for more celebration stories, help and information, and to donate or set up regular donations or online fundraising.





